Epidermolysis Bullosa (Butterfly Children disease) is a rare genetic disorder causing extremely fragile skin that blisters and tears easily, often leading to chronic wounds, infections, nutritional problems, and deformities.
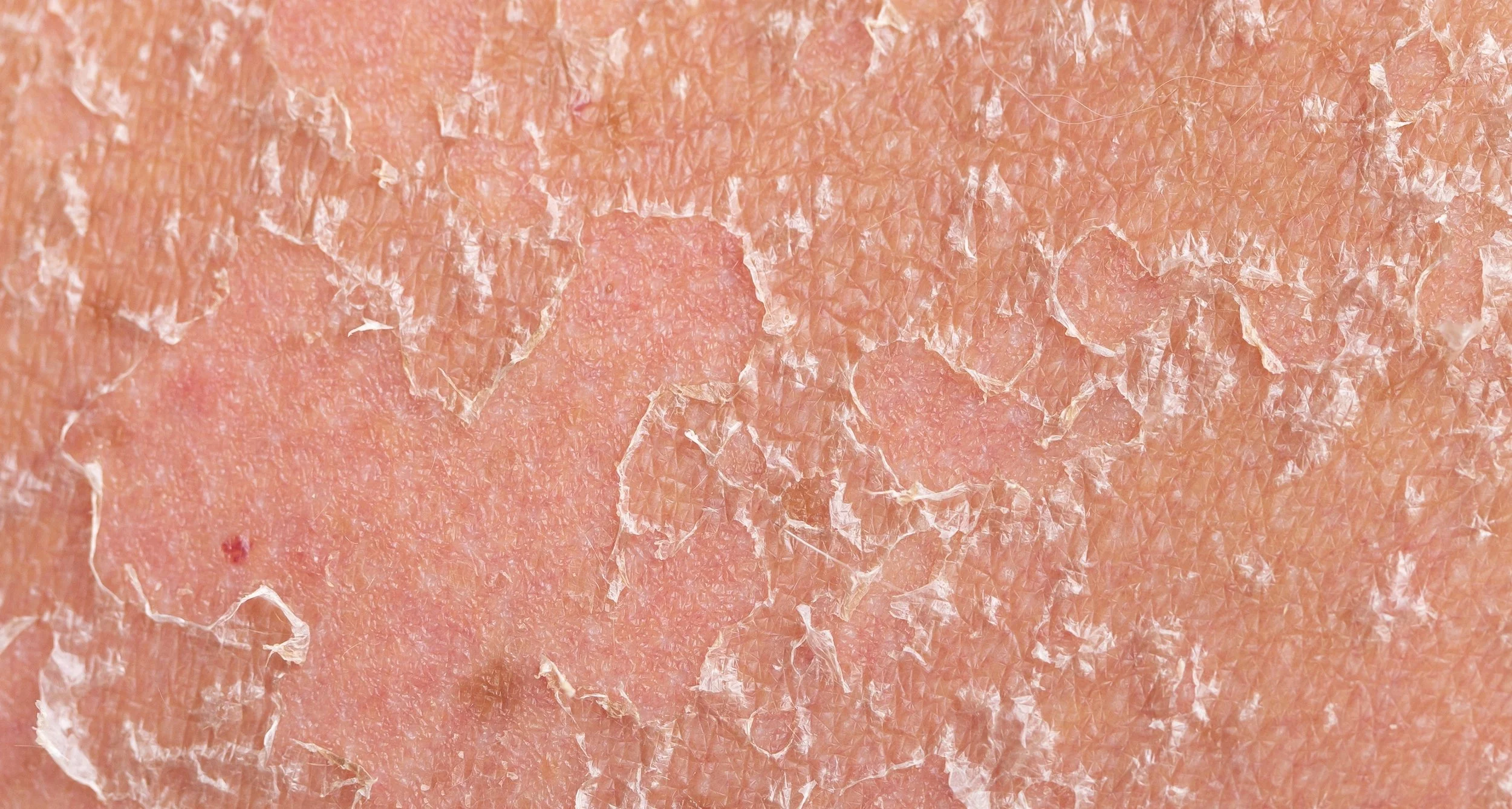
Lamellar ichthyosis treatment is mainly supportive care from birth, including incubator care, fluid management, and close monitoring to prevent skin infection, eye damage, breathing problems, and dehydration.
Lamellar Ichthyosis is a rare genetic skin disorder in which babies are born with thick, tight, armor-like skin that can cause breathing, feeding, movement, and eye problems.
Candidiasis (yeast infection) is a common fungal infection in children under 3 years old, causing red moist rashes in skin folds or white patches in the mouth, and is treated with good hygiene and antifungal medications such as Gentian Violet or Nystatin.
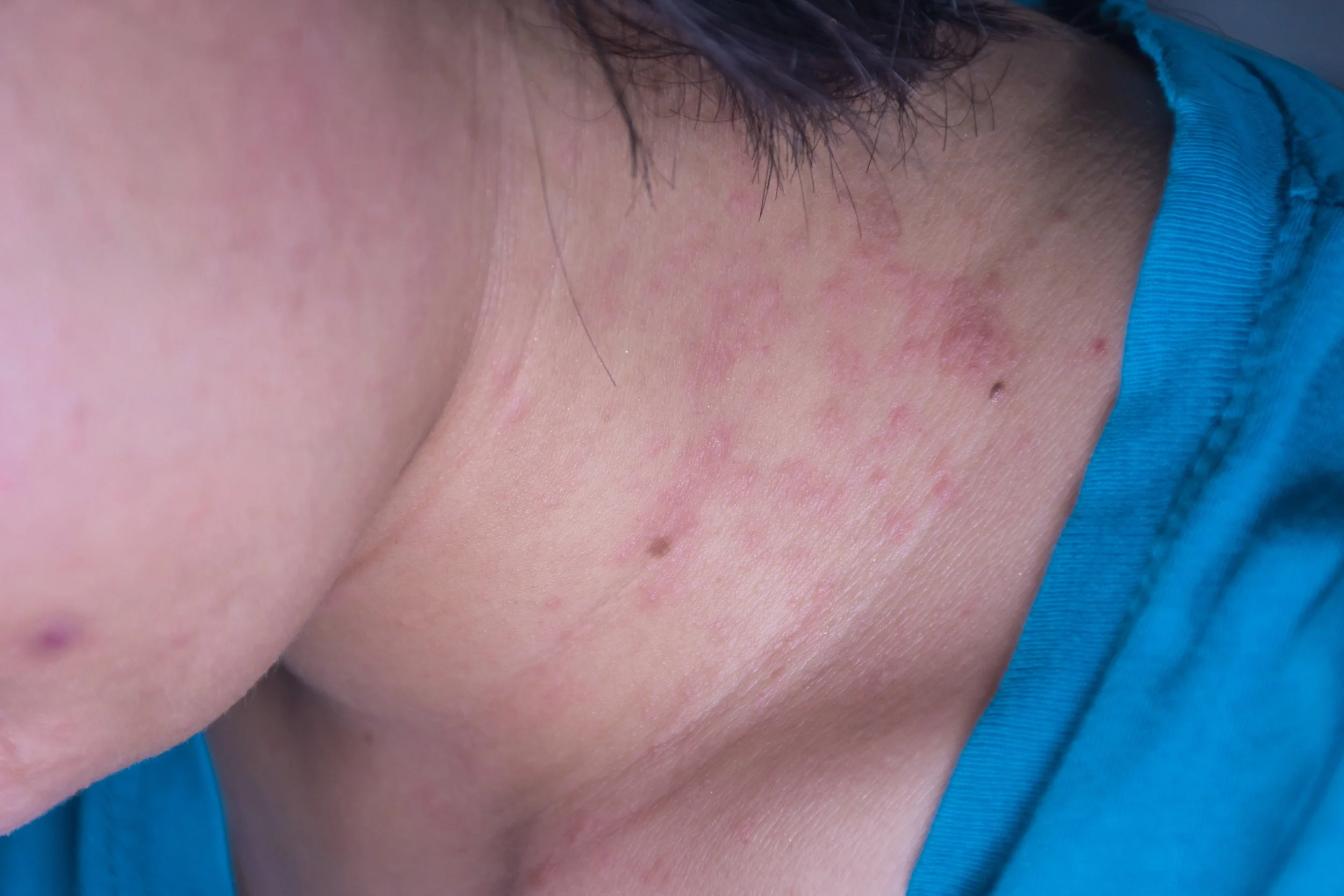
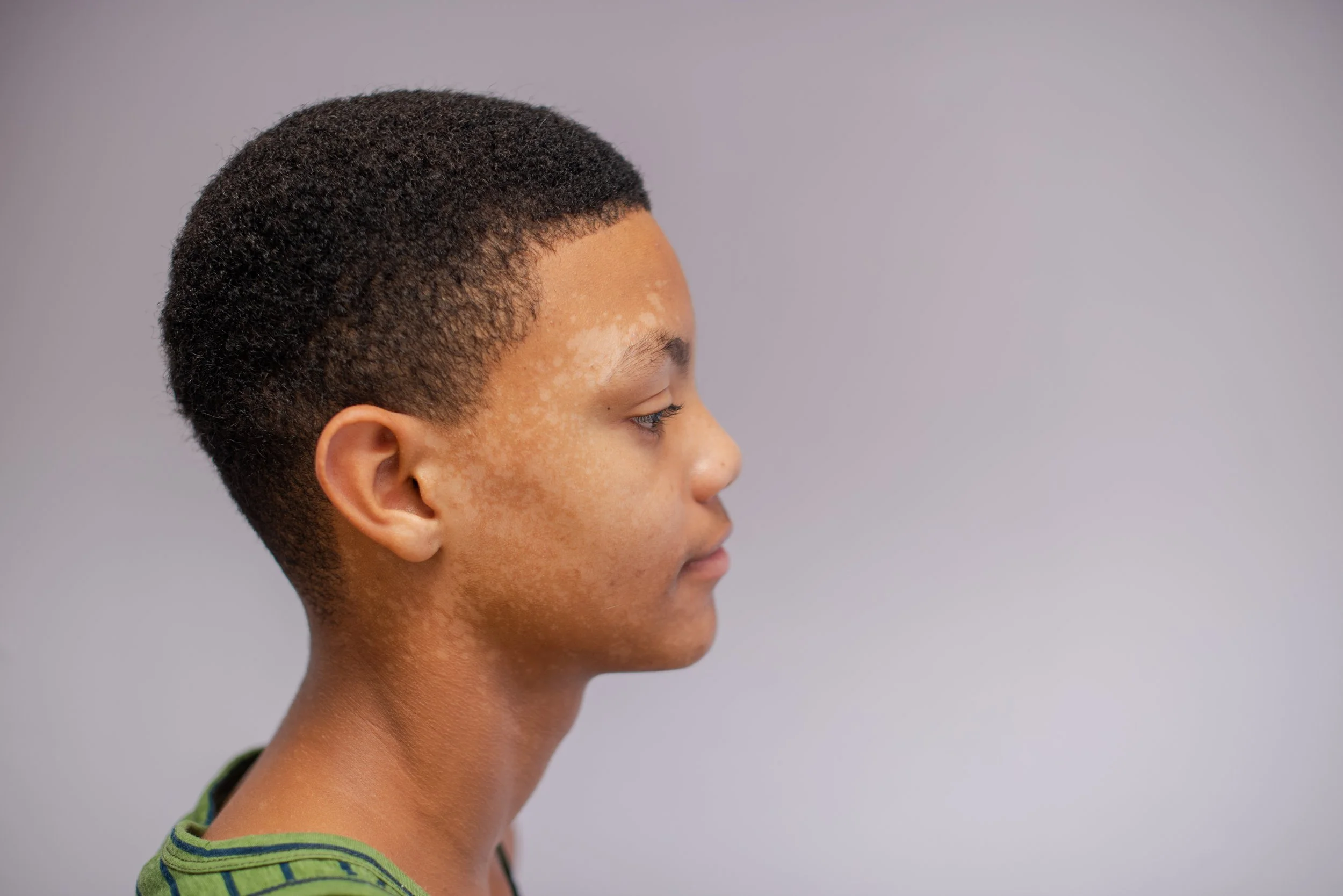
Tinea versicolor treatment aims to control the fungus and prevent recurrence through antifungal medications and proper hygiene, including keeping the skin clean, dry, and well-ventilated.
Tinea versicolor is a common fungal skin infection causing scaly patches of varying color on the body, often triggered by heat, humidity, and excessive sweating, and diagnosed through skin examination or special light/microscope tests.
For skin fungal infections, use antifungal creams, while scalp infections may require oral medication and medicated shampoo to prevent spreading.
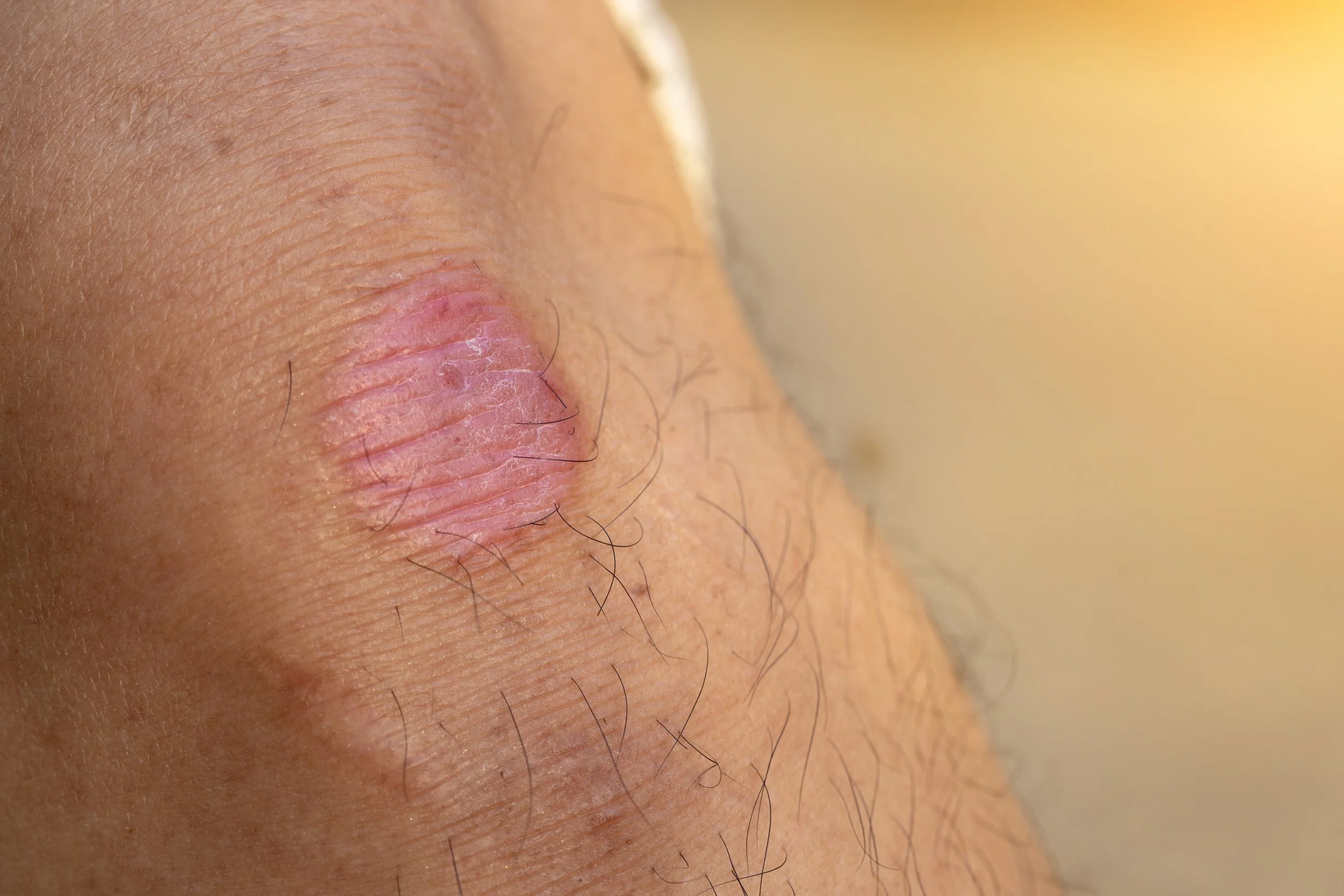
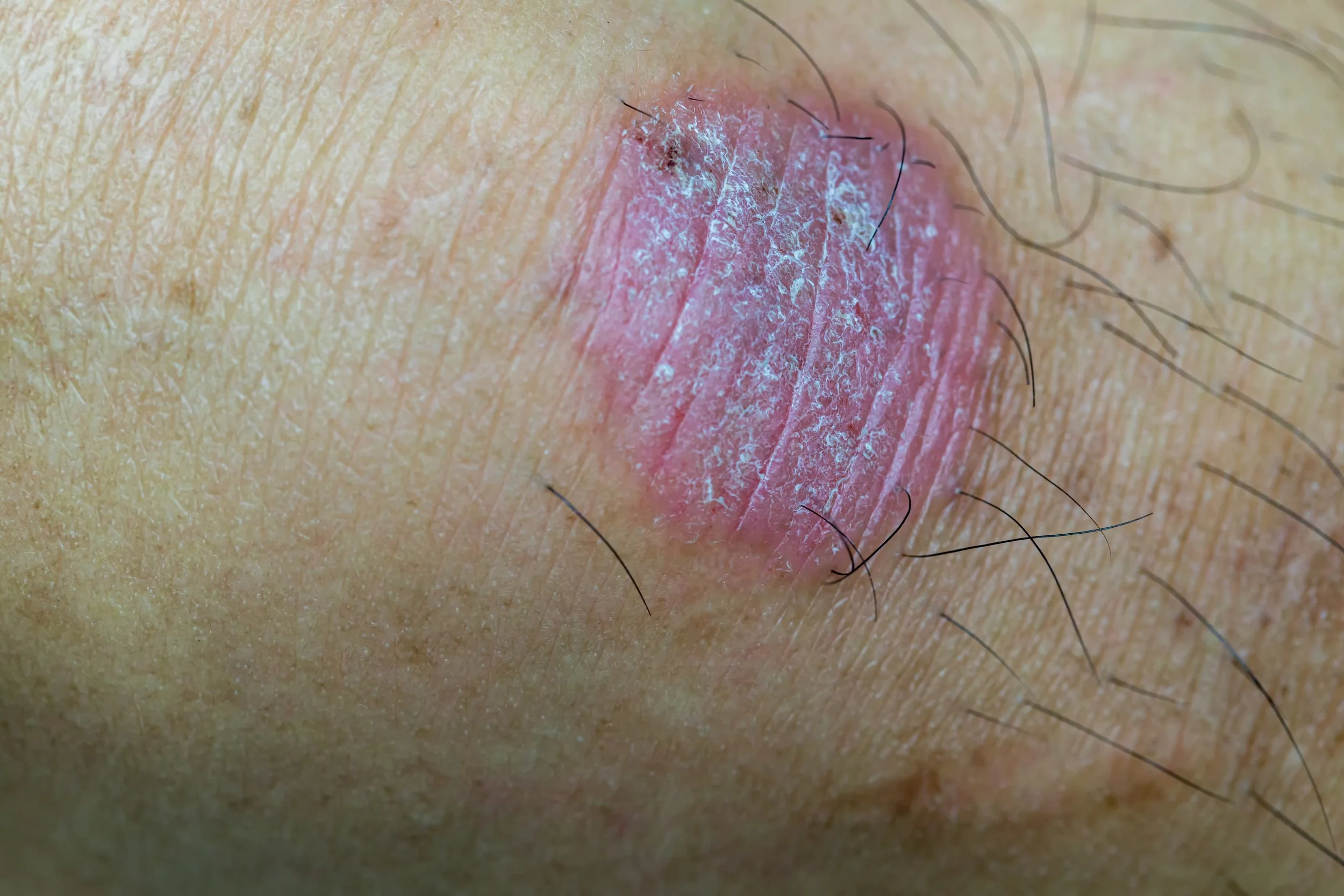
Dermatophytosis is a contagious fungal skin infection causing itchy, ring-shaped red scaly patches, diagnosed clinically and confirmed by KOH examination or fungal culture.
Common fungal infections in children are treated with antifungal medications and good hygiene, and medical attention is needed if symptoms are severe or do not improve.
Superficial fungal infections in children are mainly caused by Candida, Tinea versicolor, and Dermatophytosis (ringworm), which spread through skin contact, shared items, pets, and humid environments.
Hand, Foot, and Mouth Disease is treated with fever medicine, plenty of fluids, soft foods, and rest, while prevention includes handwashing, avoiding shared items, cleaning toys, and staying home when sick.
Hand, Foot, and Mouth Disease is a common viral infection in young children that spreads easily through contact with bodily fluids, causing fever, mouth sores, and rashes on the hands and feet, with rare but serious complications in some cases.
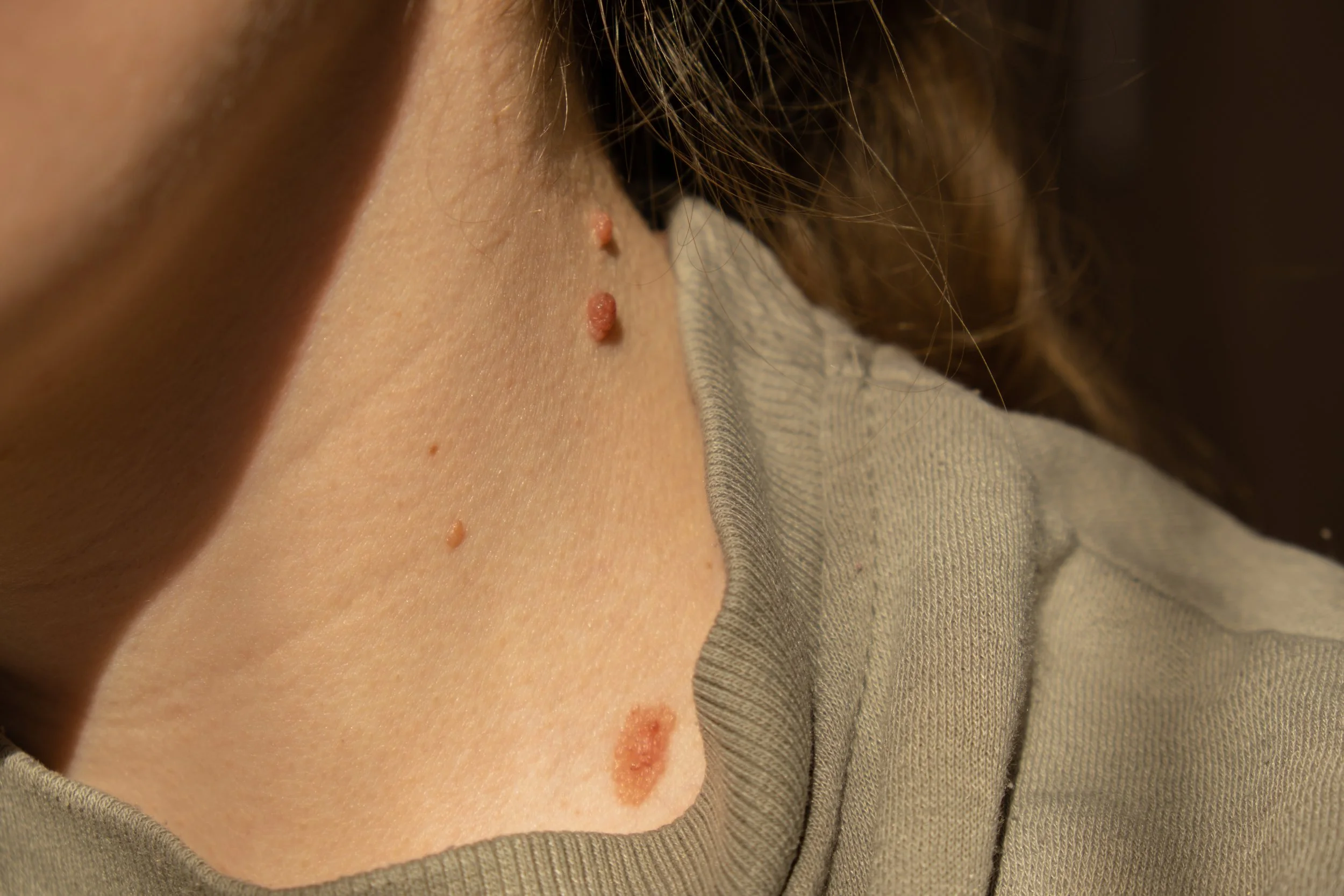
Warts are caused by the Human Papillomavirus (HPV), spread through skin contact or shared items, and usually appear as rough, hard bumps on the hands, feet, around nails, or face, which are mostly harmless but may need medical attention if painful or spreading rapidly.
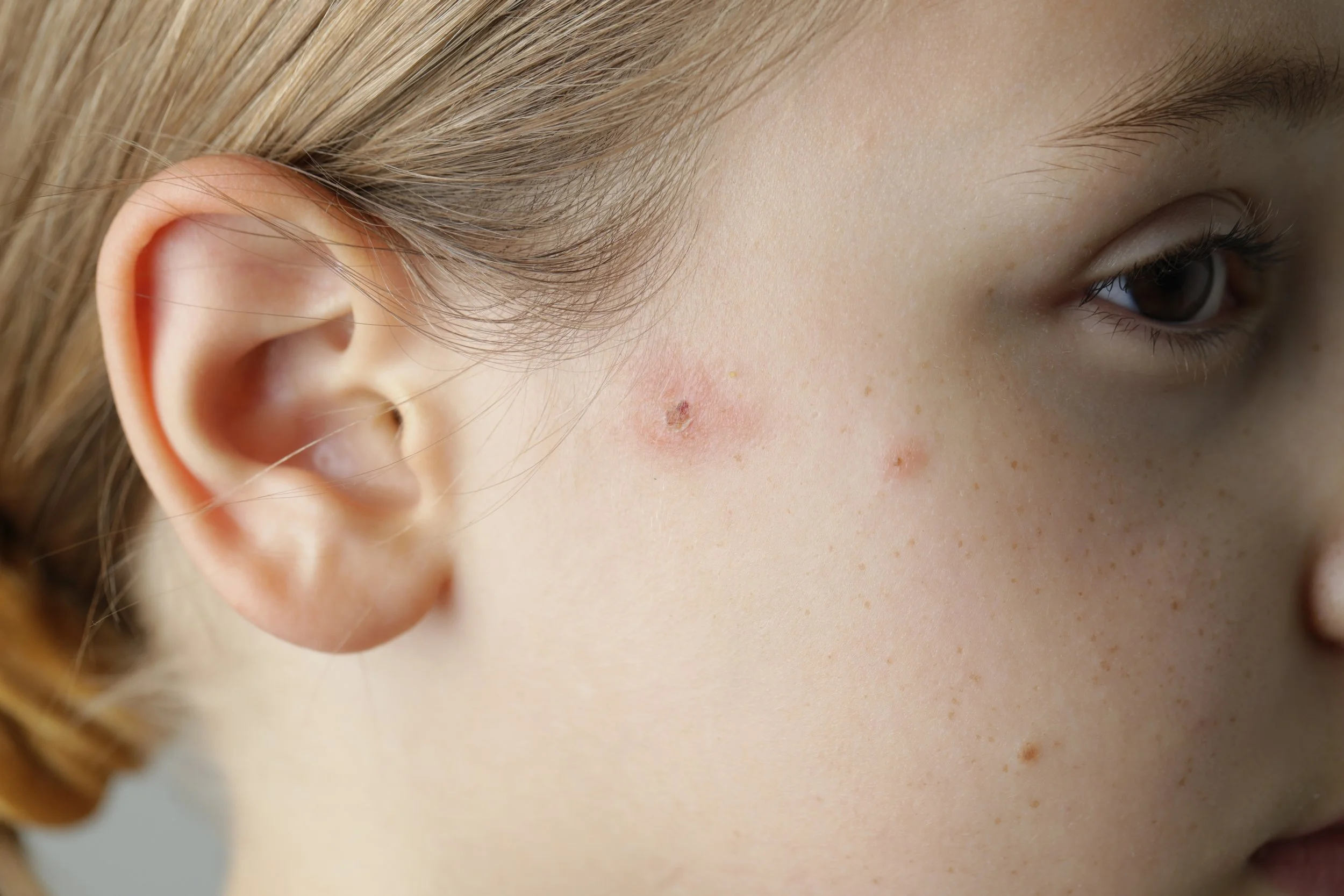
Molluscum contagiosum can be treated with topical medications, cryotherapy, curettage, or laser removal, while avoiding scratching and sharing personal items to prevent spread.
Molluscum Contagiosum is a contagious viral skin infection common in young children, causing small pearly bumps with central dimples that usually resolve on their own over time.
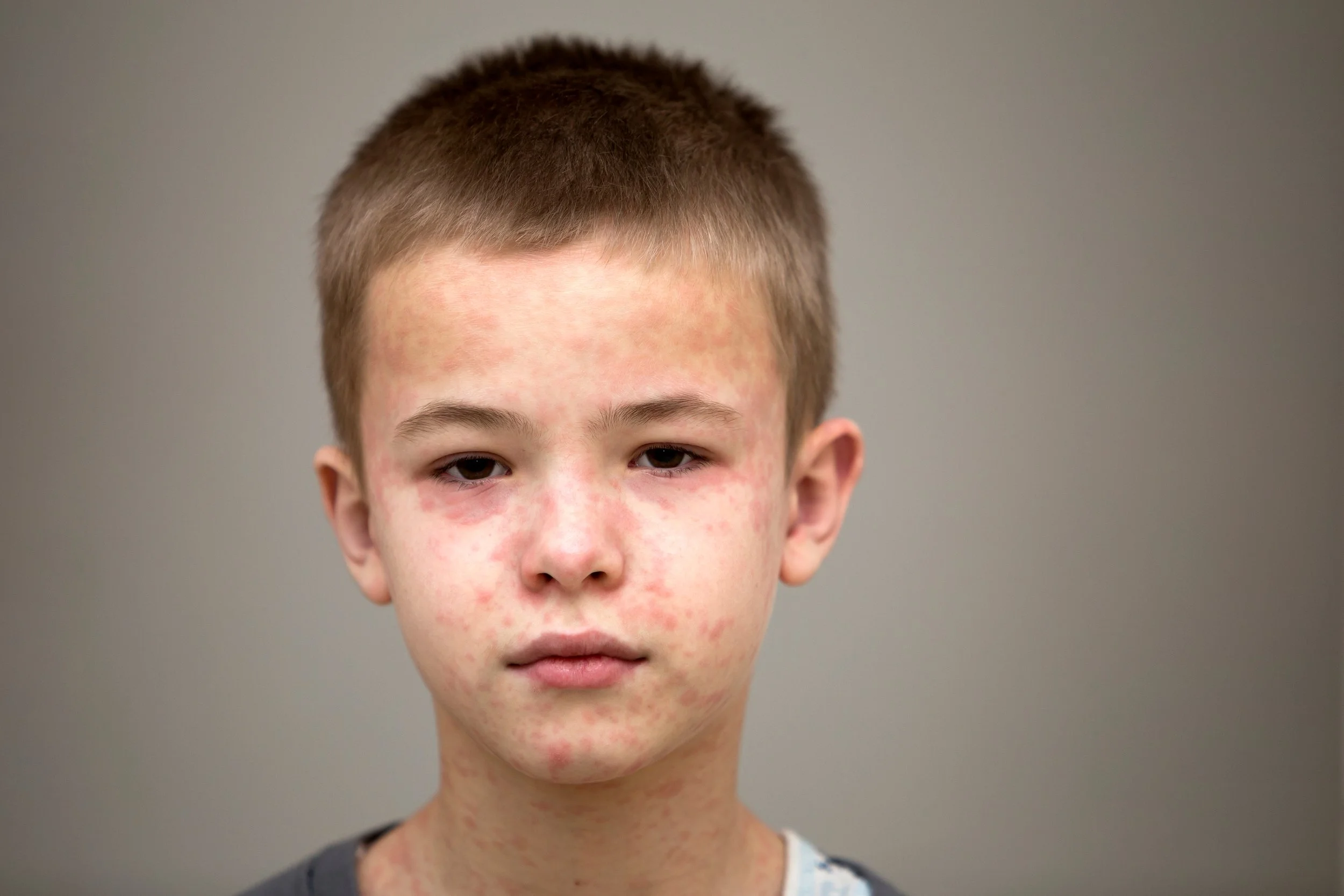
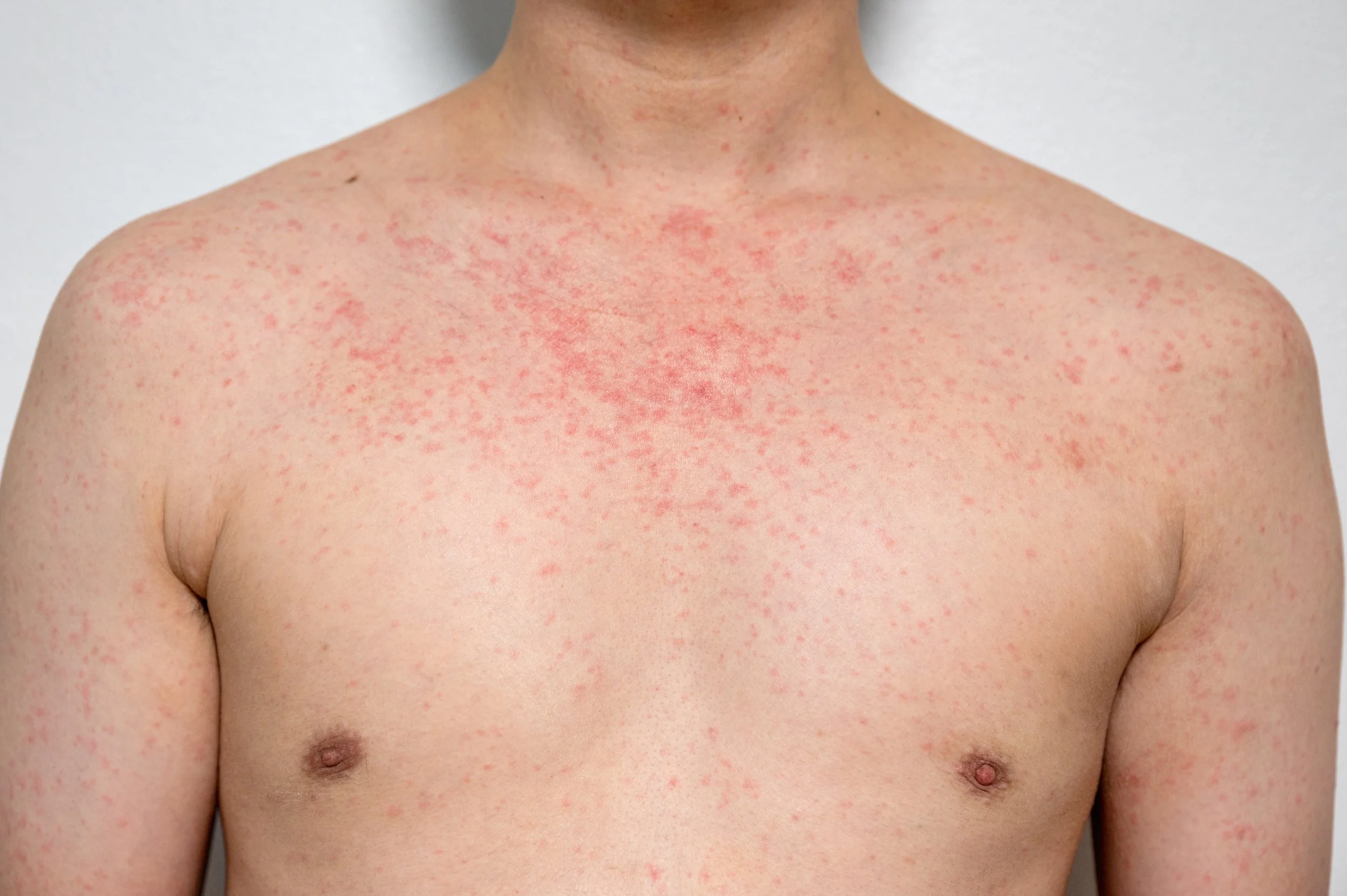
Measles is a highly contagious viral disease spread through respiratory droplets, causing fever, cough, red eyes, and rash, with potentially severe complications that can be effectively prevented by the MMR vaccine.
Roseola Infantum is a common viral illness in children under 2 years old, causing 3–5 days of high fever followed by a pink rash that resolves on its own with supportive care.
Herpes zoster (shingles) is a reactivation of the varicella-zoster virus causing painful, one-sided blistering rash and can spread through direct contact, with serious complications requiring medical attention if affecting the face or nerves.
Most people gain lasting immunity after Varicella, but the virus can remain dormant and later reactivate as Herpes Zoster; vaccination and proper care help reduce risks and complications.
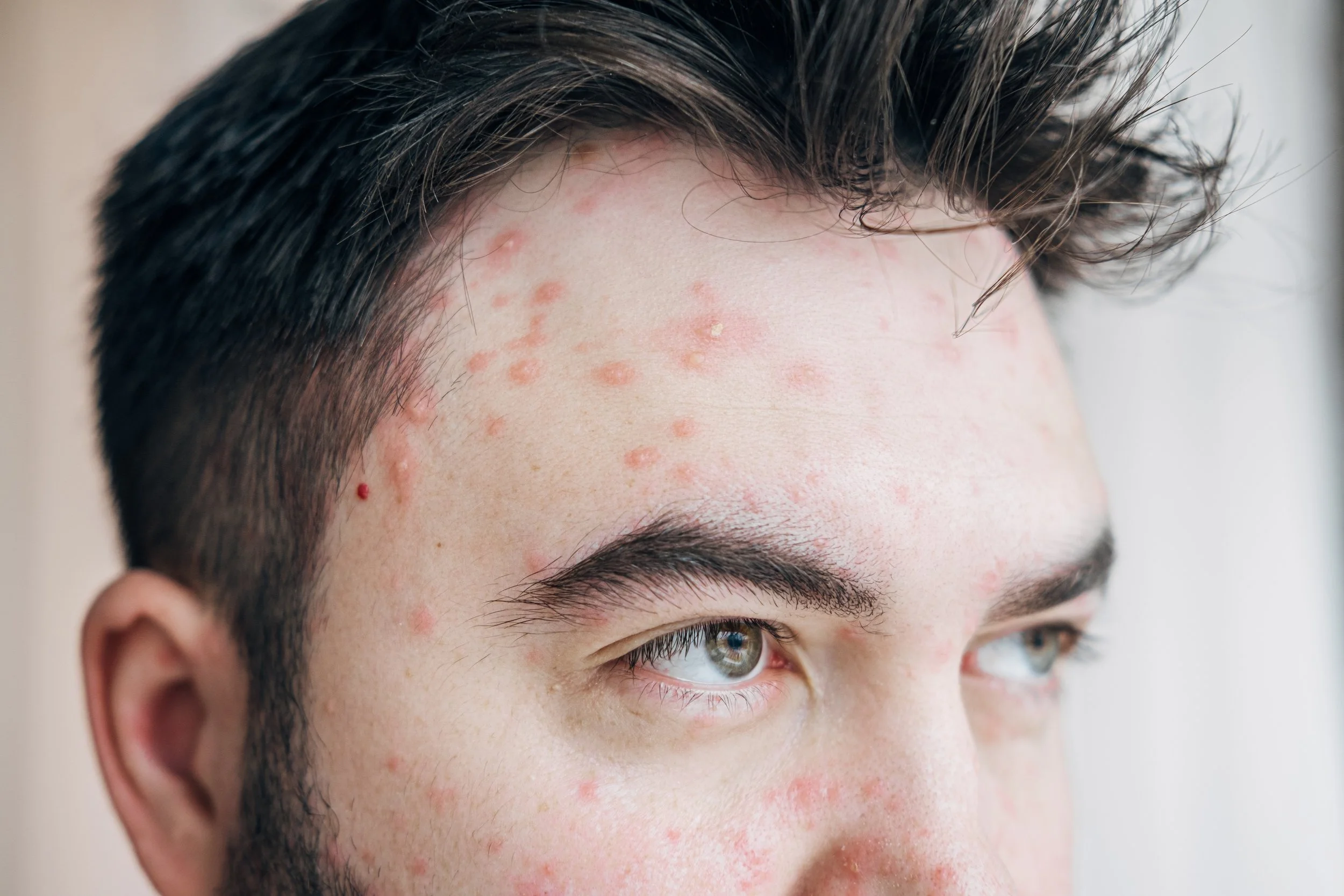
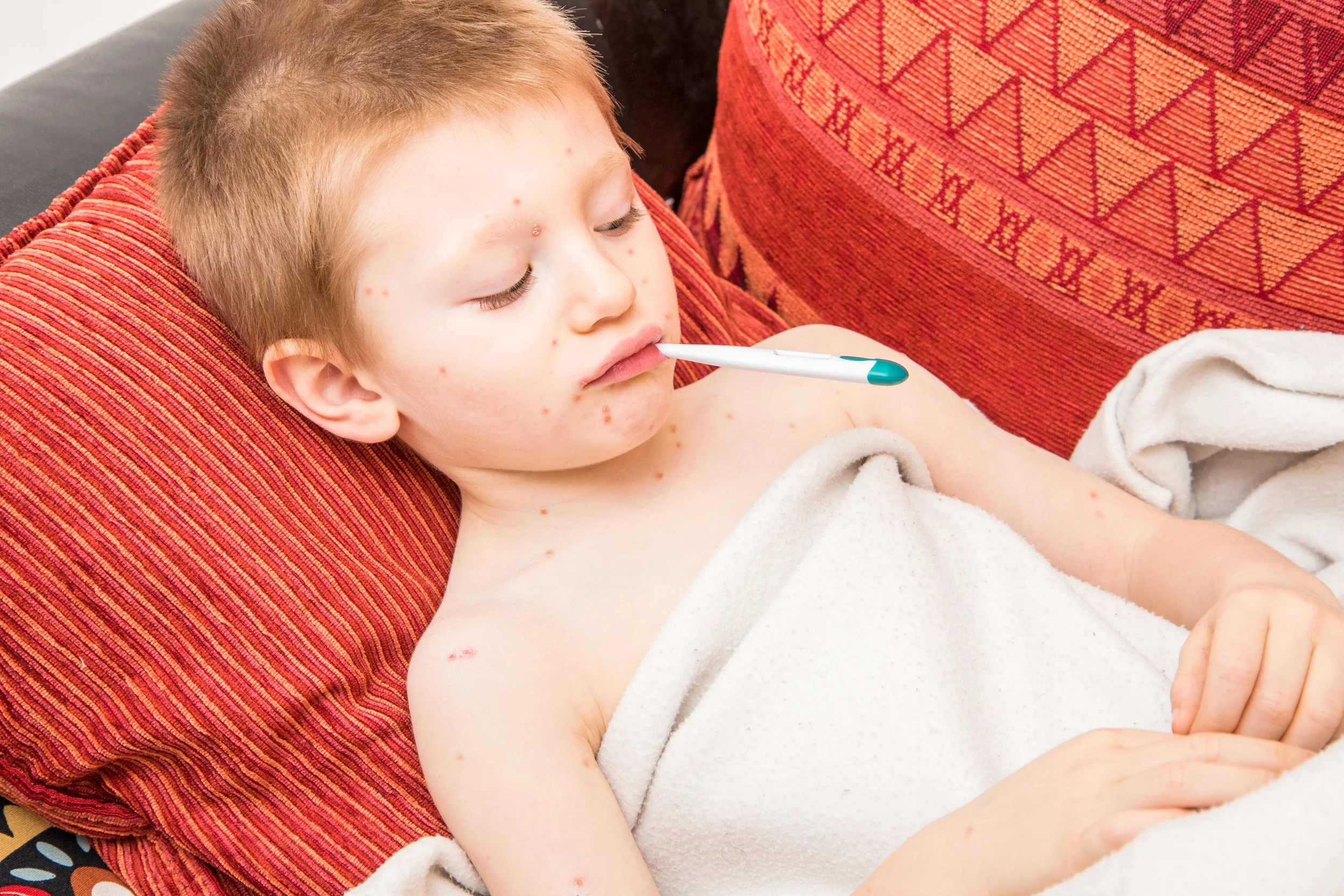
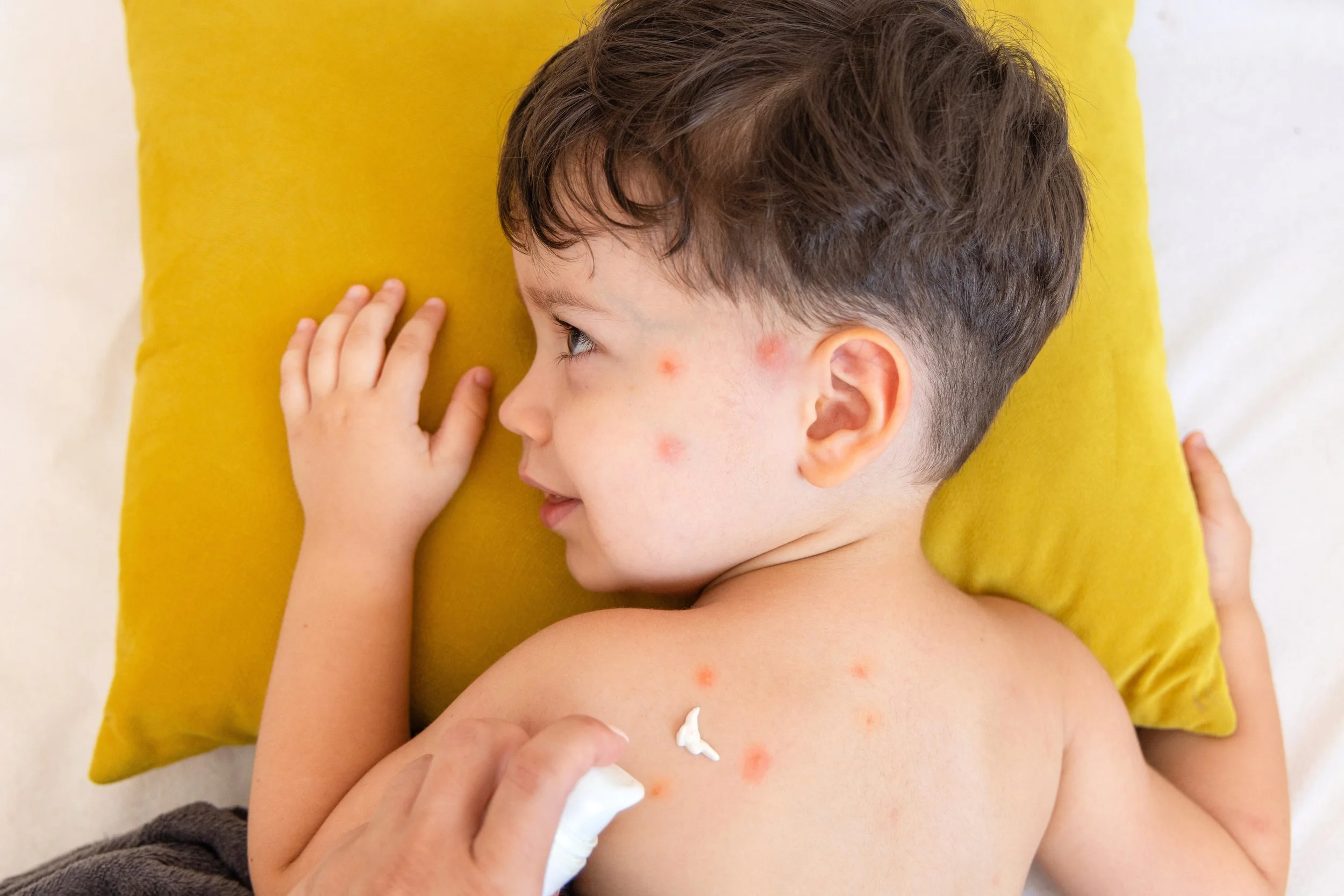
Varicella (chickenpox) is a highly contagious viral infection causing fever and itchy fluid-filled rashes in multiple stages, usually self-limiting but sometimes requiring antiviral treatment in high-risk patients.
Prompt diagnosis and antibiotic treatment of erysipelas and cellulitis are crucial to prevent severe complications like bloodstream infection, especially in high-risk groups.
Erysipelas and cellulitis are bacterial skin infections (commonly caused by Group A Streptococcus, Staphylococcus aureus, and Haemophilus influenzae) that enter through skin breaks, causing rapidly spreading red, swollen, painful lesions, especially in infants, young children, and the elderly.
Scarlet fever is a bacterial infection in young children causing fever, sore throat, strawberry tongue, and a sandpaper-like rash, treated with antibiotics to prevent serious complications.
Treatment of Impetigo includes oral and topical antibiotics, proper wound cleaning and care, and hygiene measures to prevent spread.
Impetigo is a contagious bacterial skin infection (commonly caused by Staphylococcus aureus) that enters through broken skin, causing fluid-filled blisters that turn into pus and yellow crusts, spreading easily by contact.
Paederus dermatitis is a skin irritation caused when crushed rove beetles release pederin toxin, leading to red, burning, blistering rashes that can be prevented by avoiding contact and bright lights.
Newborn skin is fragile with immature immunity, making it more prone to infection, especially when exposed to moisture, poor hygiene, or skin injury, despite the presence of normally harmless skin flora like Staphylococcus epidermidis.
After rain, jellyfish—especially fire jellyfish and upside-down jellyfish—are more likely to surface, and their stings can cause burning pain, rash, and even severe allergic reactions.
Avoid using mosquito repellents in infants under 6 months; use cautiously in young children (avoid hands, eyes, mouth, and broken skin), follow proper use to prevent toxicity, and consult healthcare professionals if unsure.